For Dr. Karim Qayumi, his first experience as a medical student in a chaotic emergency room was a wake-up call — one that has prompted the creation of a new simulation technology that will change medical education for the better.
“When it comes to transferring theoretical knowledge into practice of medicine, we have always had difficulties doing that,” said Qayumi, a University of British Columbia surgical professor and now-retired cardiovascular surgeon. “I felt this difficulty when I was a medical student [when] I got to the emergency room and I realized that books didn't teach me enough to deal with problems.”
Since that moment, Qayumi has been working to find a solution to bridge that gap between textbook education and clinical rotation programs for medical students — and he has finally found that solution in a new web-based simulation platform of his own creation called CyberPatient.
CyberPatient puts medical students in a simulated clinical setting with a digital patient, allowing them to sharpen their knowledge in a virtual space before encountering patients in an in-person setting.
Pulled from a diverse database of more than 120 real clinical cases, these virtual patients display symptoms that students must diagnose and treat accurately in real-time, including prescribing drug treatments and making surgical decisions. The online platform is interactive and animated, with an assessment tool identifying errors as they are made in order to give feedback that will help students build confidence in their treatment approach.
“The idea was to build a patient and a clinical environment in cyberspace, where a student can make all decisions, gain all competencies, without touching a real patient,” said Qayumi. “To make all the mistakes they can in a virtual environment, without consequences.”
The purpose of CyberPatient’s software technology is to make students apply what they’ve learned from their textbooks in a low-risk setting. The digital platform works to improve recall recognition memory, which then improves patient interaction.
“CyberPatient is based on the theory of transfer of learning [and so] we’re providing this environment for students to self-explore and improve their knowledge and experience,” said Qayumi. “So, it’s not just an education tool — it's also about patient safety.”
It’s a unique new technology that, if widely utilized by medical programs, Qayumi feels will help produce more confident and capable clinicians focused on improved patient care.
Creating CyberPatient: decades in the making
The technology behind CyberPatient has been more than two decades in the making, as Qayumi first began imagining the idea in the late 80s as a series of medical books.
After being overwhelmed during his first clinical rotation medical student, Qayumi realized that there was a need for something more to help students hone their skills before being exposed to the fast-paced environment of patient care.
In the late 90s, Qayumi shifted his vision from books to creating a computer program, as he thought it would better emulate the real-life experience of clinical rotations.
A partnership with UBC’s department of surgery and support from the department head at that time, Dr. Richard Finley, led to the first prototype in the late 90s, created by Qayumi’s son Tarique.
“It was very primitive, but it proved the concept that, yes, it was possible to do this,” said Qayumi.
A more advanced version of CyberPatient followed in 2000, garnering positive reviews from focus groups at UBC and in two institutions in Japan. At that time, the Internet’s speed, bandwidth and languages weren’t as advanced as the program needed them to be to mass-produce, so Qayumi and his team set to work refining the platform while they waited for the technological infrastructure to catch up with their vision.
That moment finally arrived in 2019, when CyberPatient launched worldwide in November. The new program was developed with help from the Centre for Digital Media and research grants from the National Research Council and the Industrial Research Assistance Program.
The development team’s original plan was to offer CyberPatient on a subscription basis, but instead the technology actually launched completely free to access — a decision made with the COVID-19 pandemic front of mind.
“As a Canadian company, we could not capitalize on a tragedy that humanity was having at the time,” said Qayumi. “But it has also been a huge help for us because we got an enormous amount of people into CyberPatient.”
Qayumi agreed that the pandemic’s circumstances have really helped CyberPatient break the barrier in terms of introducing his tech to the education sector, and piqued the interest of medical educators across the world. It also served as an informal beta test, allowing participants to provide feedback that has enhanced the platform with added features and functionalities.
CyberPatient’s digital premise means that in a world of reduced physical contact, medical students can still practice clinical skills without interacting with real patients or needing access to specialized equipment.
Over 300 institutions in 125 countries have signed up to use CyberPatient since its launch, and Qayumi is hoping that this initial success will catapult the technology into use in even more medical training programs in the future.
How CyberPatient is changing the future
Qayumi has always envisioned CyberPatient as an advancement to support the core values of medical education delivery. The digital platform is intended to revolutionize how medical students develop memory responses during treatment, by allowing them to learn from their mistakes on digital patients first.
Simulation programs aren’t a new concept in the world of medical training, said Qayumi, but CyberPatient does have a number of features that set it apart from other techniques currently in use.
The technology includes cases from a range of disciplines in one database, which are then presented using interactive animated avatars with an audio-visual platform. Other programs may focus on just one discipline or present cases strictly via text or by using non-animated images.
“Our platform is fully animated and fully provides a simulation, as far as technology allows. It's way ahead of everybody else, in respect to bringing in a simulated patient with interactivity,” said Qayumi.
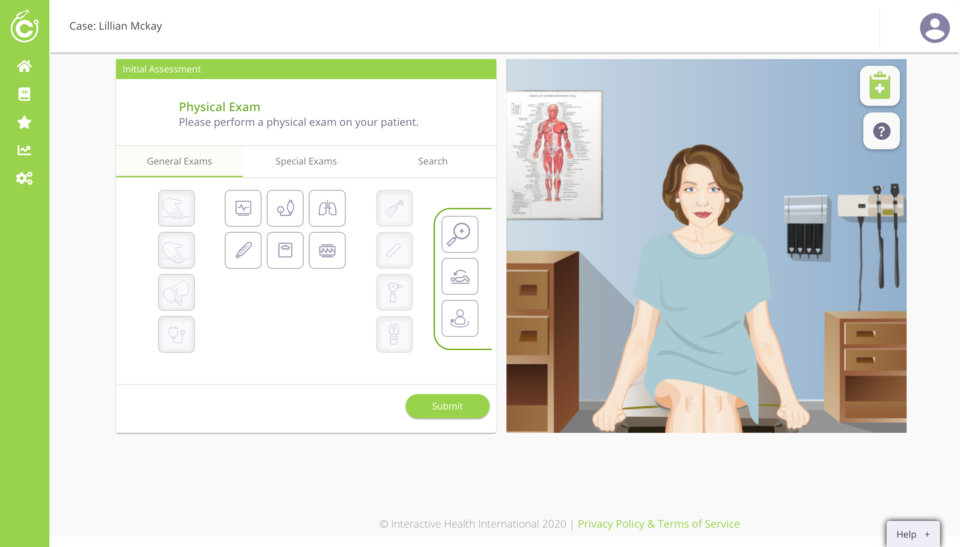 CyberPatient uses interactive patient avatars to allow students to test their clinical skills in a low-risk environment, and is the only simulation platform on the market currently using this type of audio-visual engagement. By (supplied)
CyberPatient uses interactive patient avatars to allow students to test their clinical skills in a low-risk environment, and is the only simulation platform on the market currently using this type of audio-visual engagement. By (supplied)Hands-on programs sometimes utilize mannequins with limited interactive functions or rely on live actors to pretend they are a patient experiencing symptoms. But, as Qayumi explained, these types of methods are often restricted by time and location constraints, and sometimes even budget limits.
In comparing these methods, Qayumi said that CyberPatient offers a more accessible option at a much lower price tag than mannequins or actors, while still maintaining the interactive quality that makes both types of training simulations successful.
Patients are also more available on CyberPatient’s digital platform, meaning students are able to easily familiarize themselves with more different types of diagnoses, without potential roadblocks like waiting for real patients to appear.
“Learning the practical side of medical education is very inefficient,” said Qayumi. “The majority of conditions you want students to gain experience with often stay in that level of theory, never translate into practice, so [CyberPatient] is the solution we have proposed.”
CyberPatient also takes students through the entire process of clinical care, from the emergency room or doctor’s office visit through to recovery, for each case included in its database.
“Not a lot of platforms out there cover that whole thing. They cover maybe one part [of the process] or one area of medicine,” said Qayumi. “They don’t bring a blanket solution, from A to Z, for all diseases and that’s a major difference.”
There is even a cost-awareness aspect built into the software, prompting students to consider treatment solutions that may be less expensive but still equally effective, to promote a lower-cost approach.
“This is the only tool in the market that would train students for cost-awareness because as a student, we never think about how much it's going to cost to do another X-ray or MRI, or keep a patient in hospital for another day,” said Qayumi. “But this program actually does bring cost awareness [into play] which also improves patient safety, reduces medical errors.”
In terms of assessment, CyberPatient’s intelligence system considers knowledge, time and cost as factors when judging a user's performance, said Qayumi, which helps students address their strengths and weaknesses more effectively.
A study published in the British Journal of Medical Education in 2006 found that CyberPatient’s interactive delivery is more effective than textbook learning, especially for students who struggle with classroom-based learning.
A 2020 survey of students from Kazan Federal University in Tatarstan further confirmed the technology’s popularity.
“Ninety per cent [of students surveyed] believe CyberPatient has a big impact on them. They learn better. It was very intuitive. They could use it easily, and they like it very much,” said Qayumi.
Another study also published in 2020 also showed that CyberPatient is as effective as the standardized patient method using actors, but is significantly less expensive and more cost-efficient.
Looking ahead to the future
The platform is only continuing to improve, said Qayumi, as developers are working on a number of goals to further expand CyberPatient’s technology in the future.
Since the free-to-access launch, the development team has already received feedback from users that has led to big changes. This includes improvements that made the user interface more friendly, and an update to include international medical standards in addition to North American standards, to support the international community using the technology.
There has been more interest in the simulator from professors than was originally expected, which has led to an expansion of CyberPatient’s dashboard.
Since CyberPatient was initially envisioned as a student-centred tool, it was developed to be primarily utilized by students as a supplement to their other studies. But following the booming success during the free access period, developers have since introduced a learning management system that allows professors to choose what content their students are learning.
“Lots of universities came back to us and said, we want to be in control of the education environment,” said Qayumi. “That was one of the biggest innovations for CyberPatient.”
 Students at UBC and over 300 institutions world-wide are already utilizing the technology in addition to other traditional learning methods, and they’re offering positive feedback on the industry-altering simulator. By (supplied)
Students at UBC and over 300 institutions world-wide are already utilizing the technology in addition to other traditional learning methods, and they’re offering positive feedback on the industry-altering simulator. By (supplied)And even more new features are already in the works, said Qayumi, including integrating an AI-powered vocal component into the interface, which is being developed in partnership with the National Research Council of Canada. The addition would round out the interactive nature of the program.
There are also plans to expand CyberPatient’s database to include training modules for nursing students, as well as an assessment method to measure practical skills for students entering the residency portion of their program, like communication with family or medical team members.
“Team training is another huge gap in medical education because we are all trained separately but when we come into the hospital, we have to work as a team, and that dynamic sometimes creates problems,” said Qayumi. “So we’re developing the technology to do that team training online.”
He is also working on developing partnerships with accreditation and regulatory bodies — such as the Royal College of Physicians and Surgeons of Canada, American Association of Medical Colleges, the Educational Commission for Foreign Medical Graduates, and others — to provide CyberPatient as a tool to aid with the maintenance of competency for physicians, specifically in remote northern territories.
Qayumi said that although access to CyberPatient is limited to users with a computer, part of his goal is to keep the platform simple — meaning no extraneous equipment or programs necessary to utilize the technology.
“We are trying to be as simple as possible, as fast as possible and as less expensive as possible, to [make CyberPatient] reachable,” said Qayumi.
Qayumi, in support of UBC’s vision and millennial goals, is also dedicated to delivering his technology free of charge to developing nations, as part of the non-profit program through CanHealth International, a Vancouver-based UBC spin off charitable organization.
CyberPatient is already available free to medical institutions in Ethiopia, Sudan, Afghanistan and Nepal, as well as other countries, as part of this initiative. Qayumi said he will continue to expand access to more countries and keep the technology as simple to use and as accessible as possible.
“We believe that equalization of education around the world will be able to bring positive change for all humanity,” said Qayumi.
Qayumi and his technology is also engaged in supporting the medical councils and regulatory bodies in developing countries, such as Nepal, Afghanistan, Uzbekistan, Sudan and Ethiopia, to name a few.
The cornerstone of Qayumi’s vision for CyberPatient is to improve accessibility, and so he hopes to see more institutions and practitioners utilizing this new platform to continue improving the educational experience in the medical field.
“CyberPatient is not only useful for students but also supports the faculty,” said Qayumi. “We spend less time for the same educational costs and actually improve the educational process, make it easier [for both].”
“In addition, universities will benefit from CyberPatient by replacing expensive methods of teaching and assessment for objective structured clinical examination with CyberPatient,” said Qayumi.
To learn more about CyberPatient, visit cyberpatient.ca.




